The Readiness Gap: Why Medical Students Are Knowing More and Practicing Less
Published by Symtive | Medical Simulation
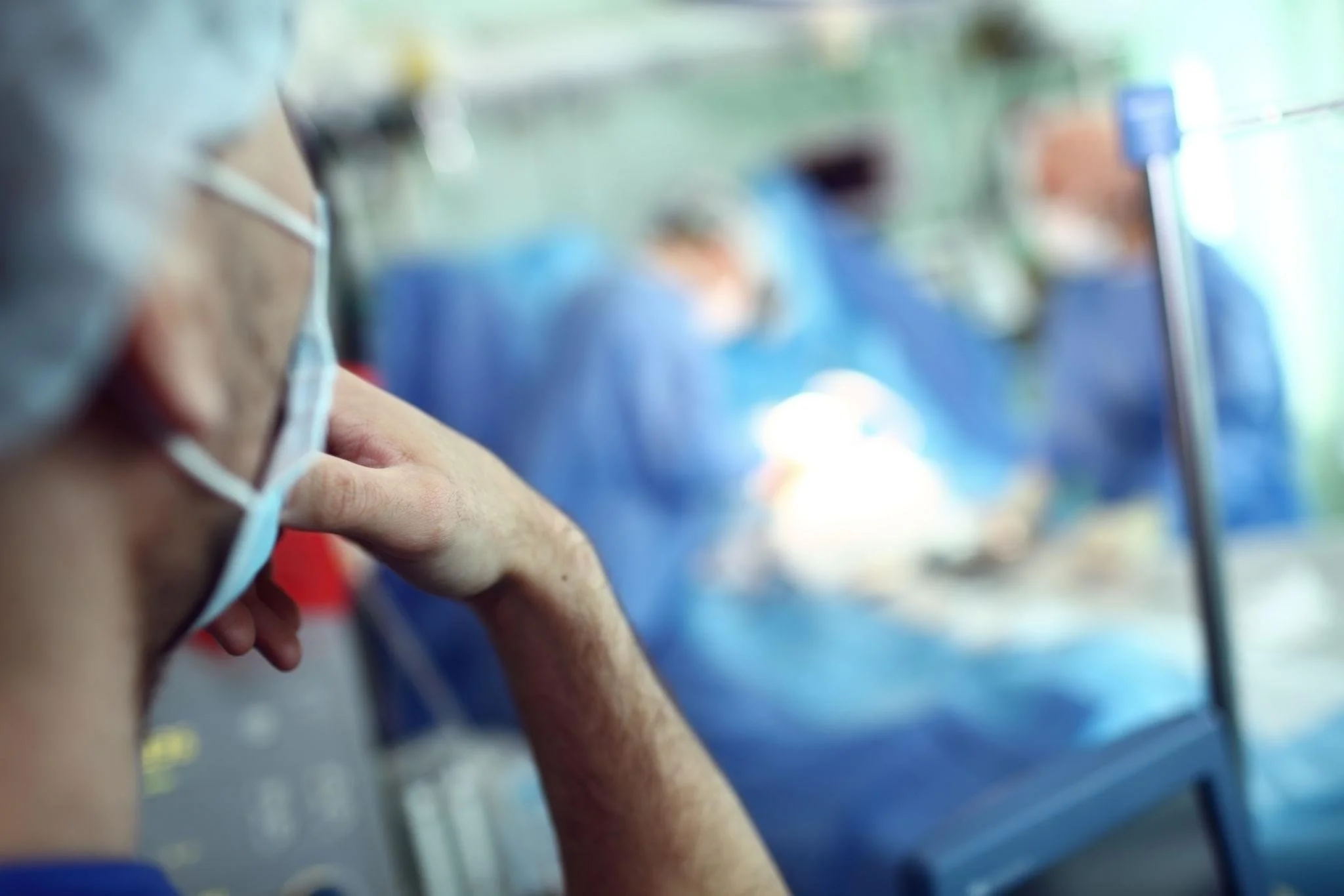
Information at your finger tips
Medical students today have access to more information than any previous generation. A question about a drug interaction gets answered in seconds. A complex procedure can be watched on demand from multiple camera angles. AI tools can walk a learner through differential diagnoses at any hour of the night.
And yet, something critical is missing.
Information is not the same as ability. And in medicine, that gap can cost lives.
Watching Is Not Doing
Consider a fourth-year medical student preparing for residency. They have spent hundreds of hours consuming high-quality educational content, video tutorials, AI-assisted case reviews, and digital textbooks. By any measure of information access, they are well-equipped.
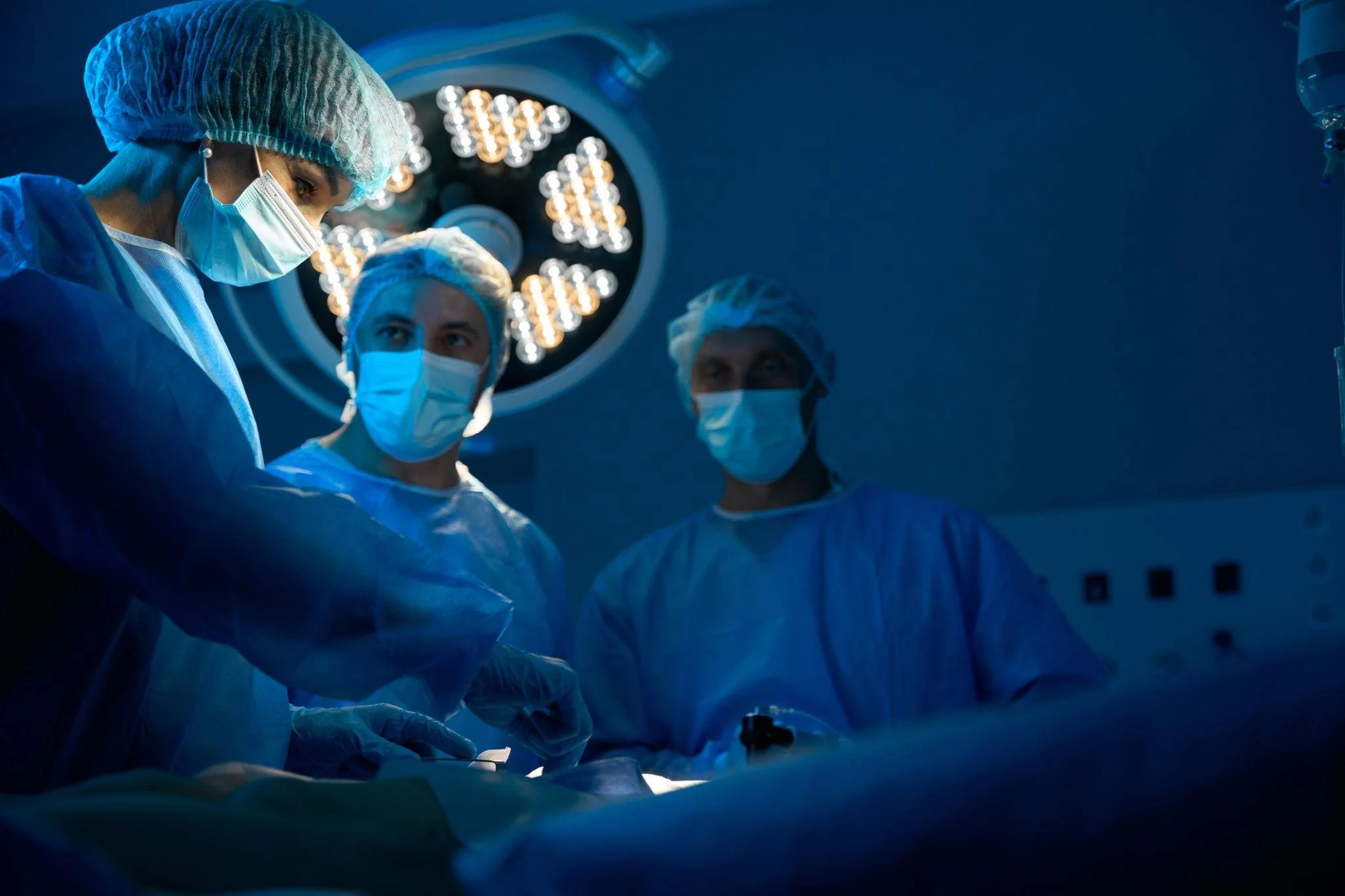
A student watching a medical procedure from observation gallery
But put them in a fast-moving clinical scenario; a patient deteriorating, a procedure needed, a decision required under pressure, and passive knowledge alone is not enough. The hands hesitate. The mind races. The performance does not match the preparation.
This is not a failure of intelligence or effort. It is the predictable result of a learning model built around consumption rather than practice.
The brain encodes procedural and clinical decision-making skills differently than it encodes facts. Repetition under realistic conditions, with time pressure, incomplete information, and real consequences, is what builds the reliable, automatic competency that clinical environments demand. Reading and watching activate very different cognitive pathways than doing.
This is the readiness gap in modern medical education: students have never known more, and many are practicing less than ever.
The Unintended Consequences of USMLE Step 1 Going Pass/Fail
One of the most significant and underappreciated forces reshaping how medical students learn came into effect on January 26, 2022, when the NBME transitioned USMLE Step 1 from a three-digit numeric score to a simple pass/fail result.
The intention was sound. Step 1 scores had become a high-stakes filter for residency applications, creating enormous anxiety and driving students to spend months in intensive test preparation at the expense of broader clinical learning. Removing the numeric score was meant to rebalance priorities and ease the transition from medical school to residency.
The data tells a more complicated story.
Pass rates dropped across every category of test taker in the year of the transition and continued declining in subsequent years. Among U.S. MD students, the first-time pass rate fell from 95% in 2021 to 91% in 2022, then to 90% in 2023. U.S. DO students dropped from 94% to 89% to 86% over the same period. International medical graduates saw the sharpest decline, falling from 82% to 74% in a single year.
Researchers studying learning behavior before and after the change found that students in the pass/fail era completed significantly less study material. They worked through fewer practice questions, built fewer review cards, and showed slower rates of improvement on practice exams compared to cohorts preparing under the scored system. One analysis noted that students were shifting their efforts toward activities that would make them competitive by other metrics; research, clinical experiences, and specialty-specific achievements, rather than deepening their medical knowledge base.
In other words, the change that was meant to reduce harmful over-preparation for a single exam may have inadvertently reduced the depth of preparation overall.
The result is a generation of students who are studying strategically to pass rather than learning comprehensively to practice. The goal shifted from mastery to the minimum threshold. And because the threshold is now binary; pass or fail, with no score to chase, there is less incentive to push beyond it.
This is not a criticism of students. It is a structural problem. When the incentive model changes, behavior follows. Medical education is now grappling with the downstream effects: students arriving at residency having cleared the bar but potentially lacking the depth of preparation that a higher numeric target once demanded.
Why Hands-On Exposure Has Also Declined
The Step 1 shift is one part of a larger picture. Several structural forces have reshaped clinical training over the past two decades:
Student getting hands-on exposure
Work hour restrictions introduced by the ACGME in 2003 capped resident hours at 80 per week, a necessary patient safety reform that nonetheless reduced the volume of cases trainees encounter over the course of their training.
Shorter hospital stays mean fewer complex cases per rotation. Patients move through the system faster, and students often see only fragments of a clinical picture.
Productivity pressure on attending physicians has, in many settings, reduced the time available for supervised trainee participation in procedures.
COVID-19 disrupted an entire cohort of clinical training, accelerating a shift toward passive digital learning out of necessity, a shift that has not fully reversed.
The combined effect is a generation of highly informed clinicians who may be under-rehearsed in the hands-on skills their roles demand from day one of residency.
The Shift to Competency-Based Education
Medical education is responding to this challenge through a broader movement toward competency-based medical education (CBME). Rather than advancing learners based on time logged or rotations completed, CBME asks a more fundamental question: can this person actually perform?
Frameworks like the AAMC's Entrustable Professional Activities (EPAs) and ACGME Milestones are redefining what readiness looks like. The goal is to make progression reflect demonstrated capability, not assumed exposure.
But competency frameworks are only as effective as the training environments that support them. Defining what competency looks like is one thing. Creating consistent, measurable opportunities for learners to build and demonstrate that competency is another, and this is precisely where simulation becomes essential.
Simulation Closes the Gap That Passive Learning Cannot
Browser-based simulation platforms give learners something that video tutorials, AI tools, and board review guides fundamentally cannot: the ability to practice, fail safely, and repeat.
A learner can watch a procedure ten times and still freeze the first time they are in the room. But a learner who has navigated that scenario across dozens of simulated experiences, each time making decisions, receiving feedback, and trying again, arrives at the bedside with something qualitatively different. Not just knowledge. Competency.
This matters even more in the post-pass/fail environment. If students are no longer being pulled toward deep mastery by the incentive of a high score, the educational environment itself needs to provide a different kind of pull. Simulation does this by making performance visible, repeatable, and measurable, creating an internal standard of readiness that a pass/fail threshold cannot.
Effective simulation training enables:
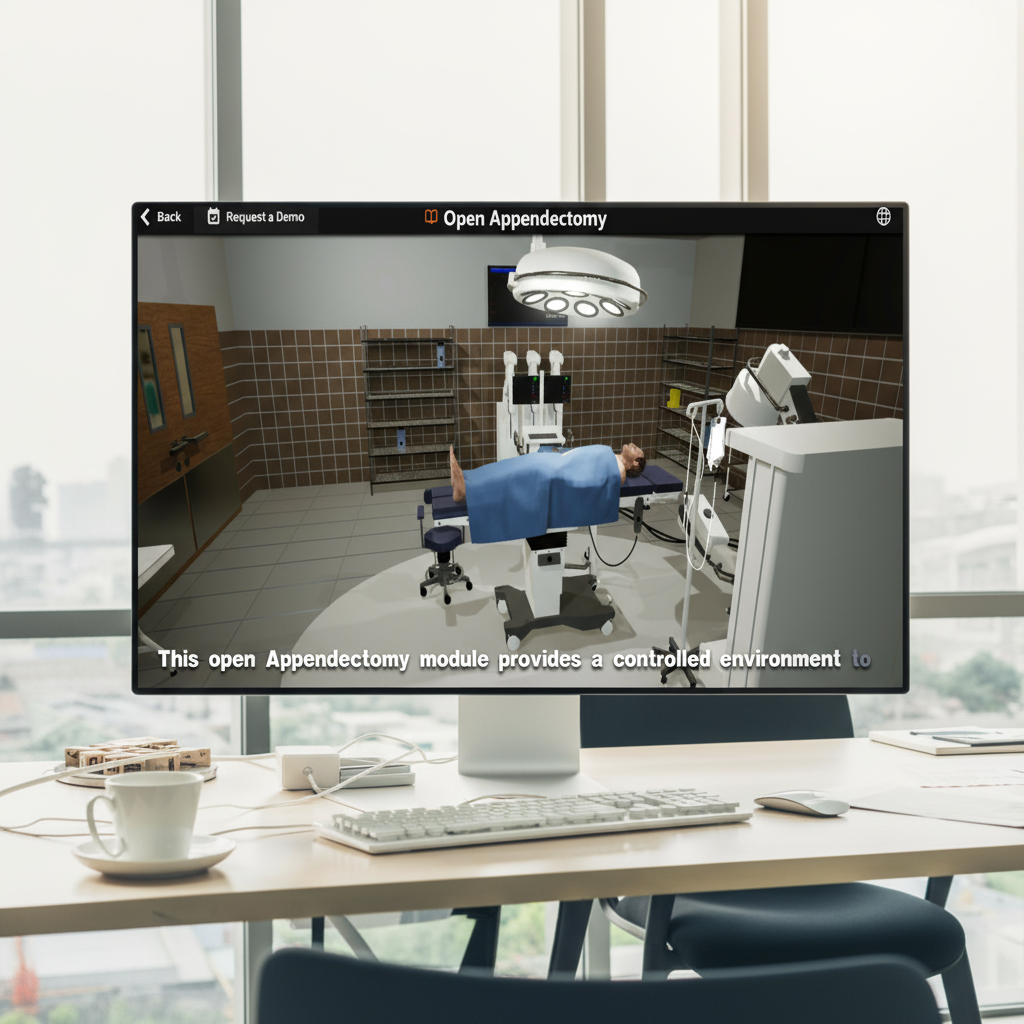
Symtive’s browser-based simulator
Repetition without risk - Learners can practice high-stakes procedures and clinical decisions as many times as needed without patient safety implications.
Realistic pressure - Scenarios replicate the time constraints, ambiguity, and complexity of real clinical environments.
Measurable performance data - Unlike passive learning, simulation captures how a learner actually performs: decision pathways taken, time to recognize clinical changes, error frequency, and improvement across repeated sessions.
Specific feedback loops - Learners and faculty can review performance objectively, making coaching targeted and actionable rather than impressionistic.
This is not about replacing clinical experience or board preparation. It is about ensuring that learners develop genuine procedural and clinical competency, the kind that does not show up in a pass/fail result but absolutely shows up on day one of residency.
Data That Actually Measures Readiness
One of the most significant advantages of simulation-based training is what it produces beyond the learning experience itself: objective performance data.
Traditional clinical assessment depends heavily on observation, which is variable, infrequent, and context-dependent. A supervisor may see a trainee in a handful of moments over an entire rotation and be asked to assess their readiness.
Modern simulation platforms change this entirely. Educators can analyze how a learner performs across dozens of scenarios, identify patterns of error that would never surface in occasional observation, and track genuine improvement over time. This moves the assessment from subjective impression to evidence of actual performance.
For program directors and accrediting bodies increasingly focused on outcomes, this is exactly the kind of documentation that demonstrates a program's commitment to producing safe, competent clinicians, and it fills a gap that the pass/fail Step 1 result simply cannot address.
The Right Tool for the Right Job
Digital learning tools each serve a purpose. AI platforms are powerful for knowledge acquisition. Video content supports conceptual understanding. Board review guides help students clear the licensing threshold.
But none of these tools gives learners practice. None of them builds the procedural fluency and high-pressure decision-making that clinical environments demand. And in a landscape where the primary licensing incentive no longer drives students toward deep mastery, the tools that actually build competency matter more than ever.
Simulation is not a replacement for the other tools in a medical student's or program's toolkit. It is the component that converts information into ability, the bridge between knowing and doing, between passing a test and being ready to practice.
Built for Medical Education
At Symtive, we build custom browser-based 3D simulation platforms for the industries where performance under pressure matters most, including medical and healthcare education.
Our simulators are accessible on any device, require no specialized hardware, and are designed to support measurable, repeatable, performance-based training. Whether you are training students on clinical procedures, medical device operation, or critical decision-making scenarios, we build simulation environments tailored to your program's specific needs and outcomes.
See what competency-based simulation looks like in practice.
Explore our medical demos at demos.symtive.com
Train Anytime, Anywhere, and On Any Device
Symtive builds browser-based 3D training simulators for automotive, aerospace, defense, medical, and industrial manufacturing. Learn more at symtive.com.