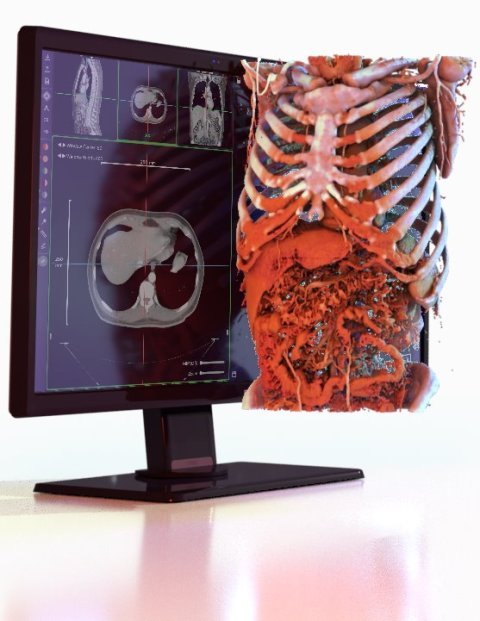
From 2D Imaging to Interactive 3D: A New Era of Clinical Visualization
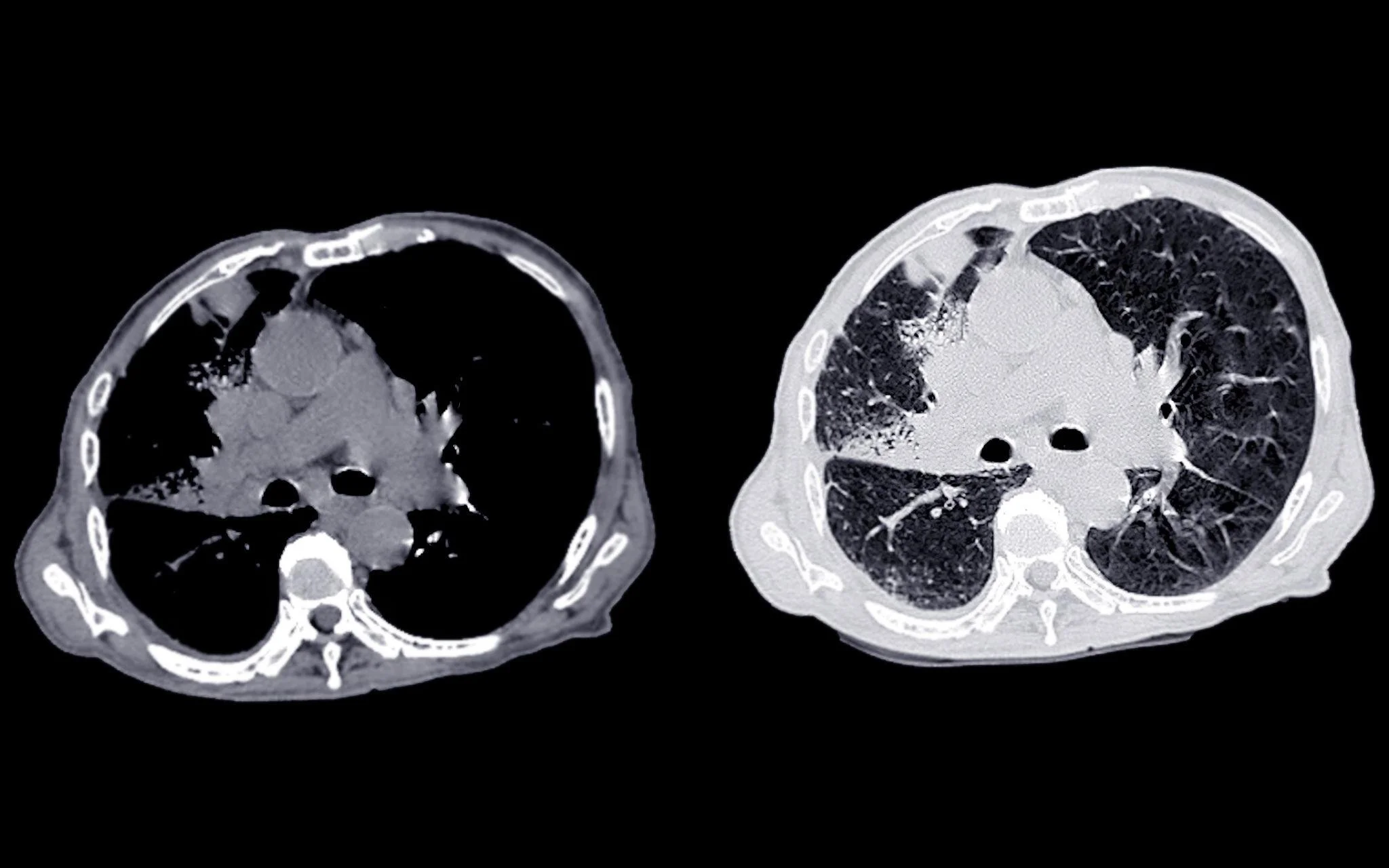
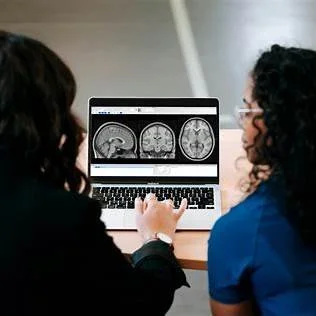
2D CT scan of brain
For decades, clinical decision-making has relied heavily on 2D medical imaging; CT scans, MRIs, X-rays, and ultrasound slices viewed on flat screens. These imaging modalities have been essential to diagnosis, treatment planning, and ongoing patient care.
However, as medical cases become more complex and care teams more collaborative, the limitations of viewing three-dimensional anatomy through two-dimensional slices are becoming more apparent. Clinicians are often required to mentally reconstruct depth, spatial relationships, and anatomical complexity from a series of static images.
Today, healthcare is entering a new era of clinical visualization; one where interactive 3D models are transforming how clinicians interpret imaging data, plan procedures, educate patients, and train future providers.
The Limitations of Traditional 2D Imaging
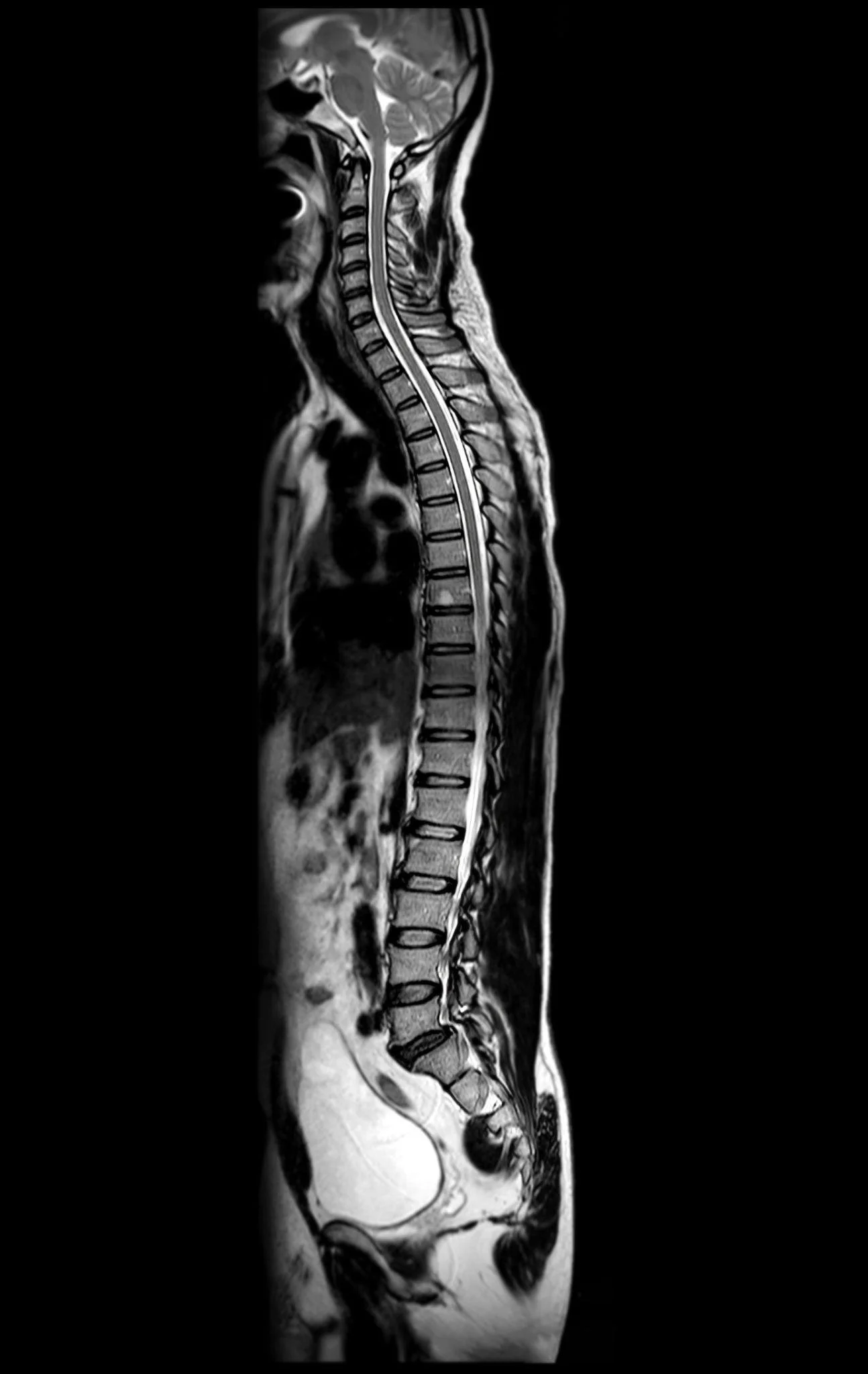
2D MRI of spine
Traditional 2D imaging remains highly precise and indispensable for diagnostics, but it places a significant cognitive burden on clinicians. Understanding complex anatomy from stacked image slices requires experience, spatial reasoning, and time.
In challenging cases, clinicians must mentally assemble multiple views to interpret:
The depth and positioning of structures
The relationship between organs, vessels, and pathology
The spatial impact of tumors, lesions, or abnormalities
The procedural approach required for treatment
While experts are skilled at this process, it can still slow interpretation, complicate interdisciplinary discussions, and make it harder to communicate findings clearly to patients and non-specialists.
These challenges are driving interest in more intuitive visualization approaches that reduce cognitive load and improve shared understanding.
The Emergence of Interactive 3D Clinical Visualization
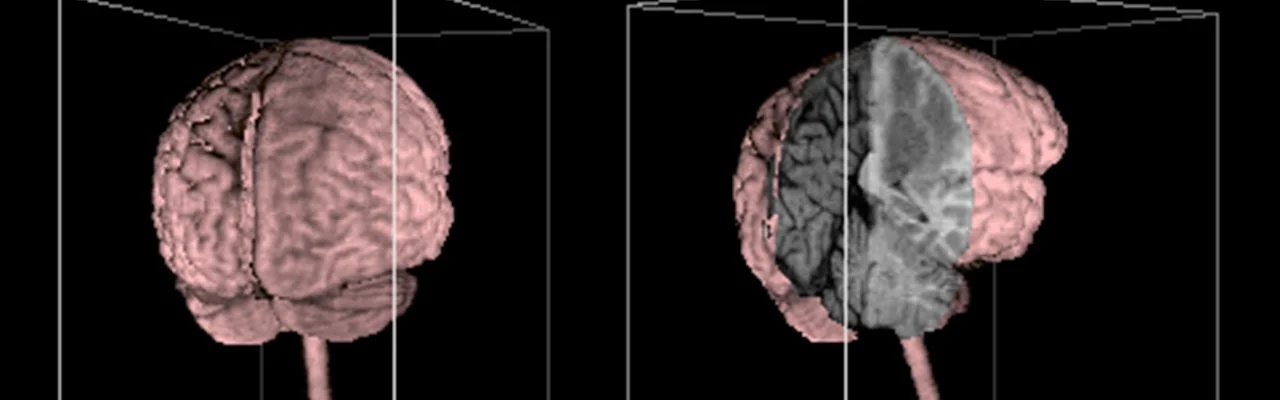
Advances in rendering technology, cloud computing, and data processing are enabling medical imaging datasets to be reconstructed into fully interactive 3D models. Instead of passively scrolling through slices, clinicians can now explore anatomy as volumetric structures in space.
Interactive 3D visualization allows users to rotate, zoom, isolate, and examine anatomical regions from any angle. This transforms imaging from a static review process into an exploratory experience that more closely reflects how anatomy exists in the real world.
Rather than imagining how structures relate to each other, clinicians can directly observe those relationships, leading to faster comprehension and more confident clinical decisions.
3D image of brain
Enhancing Clinical Decision-Making
Interactive 3D visualization is proving particularly valuable in complex clinical scenarios where spatial awareness is critical.
Pre-Surgical Planning
Surgeons can analyze patient-specific anatomy in three dimensions, helping them better anticipate procedural challenges and refine their surgical approach. Understanding exact spatial relationships between critical structures can support more precise and confident planning.
Interdisciplinary Collaboration
Modern healthcare relies on collaboration between radiologists, surgeons, specialists, and care teams. Interactive 3D models provide a shared visual reference that improves communication and alignment during case reviews and treatment planning discussions.
Patient Communication
Explaining a diagnosis or treatment plan using abstract 2D scans can be difficult for patients to grasp. Interactive 3D visualizations make it easier to show exactly where a condition exists and how it may be treated, supporting clearer, more informed conversations.
From Imaging Data to Patient-Specific Digital Models
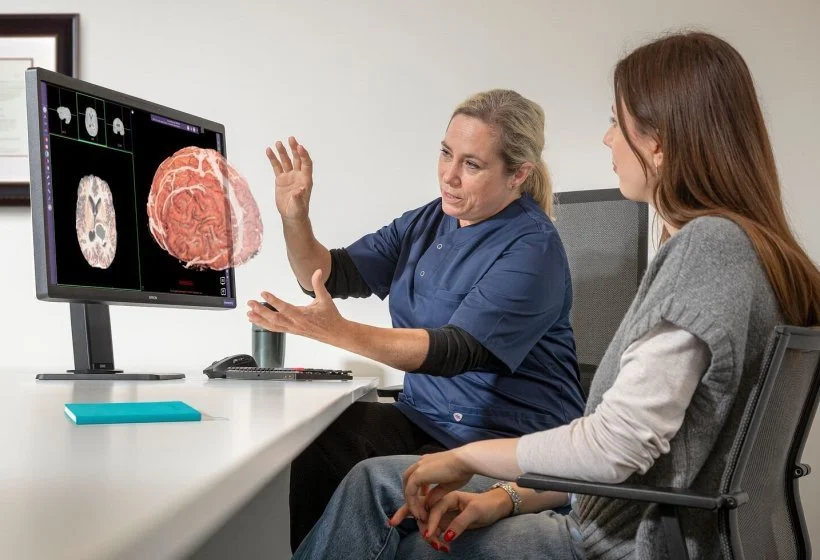
patient viewing of 3D image
One of the most exciting developments in clinical visualization is the creation of patient-specific 3D models derived directly from imaging data. These digital representations allow clinicians to examine a patient’s unique anatomy in detail rather than relying solely on generalized anatomical references.
Such models can support personalized treatment planning, procedural rehearsal, and deeper analysis of disease impact. By visualizing the exact anatomical context of a condition, clinicians can move closer to truly individualized care strategies.
This shift reflects a broader movement toward precision medicine, where treatments are tailored not just to diagnoses, but to the specific anatomical and physiological characteristics of each patient.
Transforming Medical Education and Training
The evolution from 2D to interactive 3D visualization is also reshaping medical education. Traditional learning methods; textbooks, static diagrams, and cadaver labs; remain valuable but can limit learners’ ability to fully understand complex spatial relationships.
Interactive 3D environments enable students and trainees to explore anatomy dynamically, observe physiological processes in context, and reinforce learning through repeated self-directed exploration. This creates a more engaging and intuitive educational experience that aligns with modern digital learning preferences.
Trainees can better connect theoretical knowledge with clinical application by visualizing how structures interact in real-world scenarios rather than memorizing isolated images or diagrams.
Accessibility Through Browser-Based Visualization
Another important advancement is the growing availability of browser-based 3D visualization platforms. Instead of requiring specialized workstations or installed software, clinicians and learners can access interactive models securely through standard web browsers.
3D Image
This accessibility supports:
Easier deployment across hospitals and academic institutions
Remote access for distributed care teams and learners
Reduced IT overhead and installation requirements
Consistent user experiences across multiple devices
By lowering technical barriers, browser-based visualization helps integrate advanced imaging tools more seamlessly into daily clinical workflows and educational programs.
Complementing, Not Replacing, 2D Imaging
Despite these advances, traditional 2D imaging modalities remain foundational to medical diagnostics. CT, MRI, and other imaging techniques provide the detailed data necessary to generate accurate clinical interpretations.
2D MRI image review
Interactive 3D visualization should be viewed as a complementary layer that enhances, rather than replaces, these established modalities. By combining the precision of 2D imaging with the spatial clarity of 3D models, clinicians gain a more complete and intuitive understanding of patient anatomy and pathology.
This integrated approach allows healthcare providers to leverage the strengths of both methods: detailed imaging data and immersive spatial insight.
The Future of Clinical Visualization
As computing power continues to grow and rendering technologies advance, the integration of interactive 3D visualization into routine clinical practice is expected to accelerate. Future systems will likely connect imaging data with simulation, analytics, and predictive modeling to support more proactive and personalized care.
Clinical visualization will move beyond simple image review toward dynamic environments that allow clinicians to explore, analyze, and even simulate potential treatment paths before decisions are made.
This progression represents more than a technological improvement. It signals a shift toward more intuitive, collaborative, and patient-centered healthcare experiences.
Final Thoughts
Clinical imaging has always aimed to make the invisible visible. The transition from 2D imaging to interactive 3D visualization takes that mission further by transforming static images into dynamic, explorable representations of anatomy and disease.
By reducing cognitive load, enhancing communication, and supporting personalized treatment planning, interactive 3D visualization is helping clinicians see not just more data—but a clearer picture of the patient as a whole.
As this technology continues to evolve, it will play an increasingly important role in how healthcare providers understand complex conditions, educate future clinicians, and ultimately deliver safer, more informed patient care.